Surviving the Unthinkable: Life with the Rarest Diseases

Imagine being allergic to water. Or collapsing under sunlight. These scenarios may sound fictional, but for a handful of people worldwide, they are a daily reality. When it comes to rare diseases, some are so extreme they challenge what we consider essential to human life. This blog explores a few of these medical anomalies and the resilience of those who live with them.
Table of Contents
What Are Rare Diseases?
A rare disease, also known as an orphan disease, is a medical condition that affects a very small percentage of the population. In the United States, a disease is officially classified as rare if it affects fewer than 200,000 people. These illnesses are often overlooked due to their low prevalence, which leads to delayed diagnoses, minimal research, and limited treatment options.
Rare diseases can range from mildly disruptive to profoundly disabling or even life-threatening. While some cause physical symptoms, others deeply impact mental health, social life, and basic daily routines.
1. Aquagenic Urticaria: The “Water Allergy”
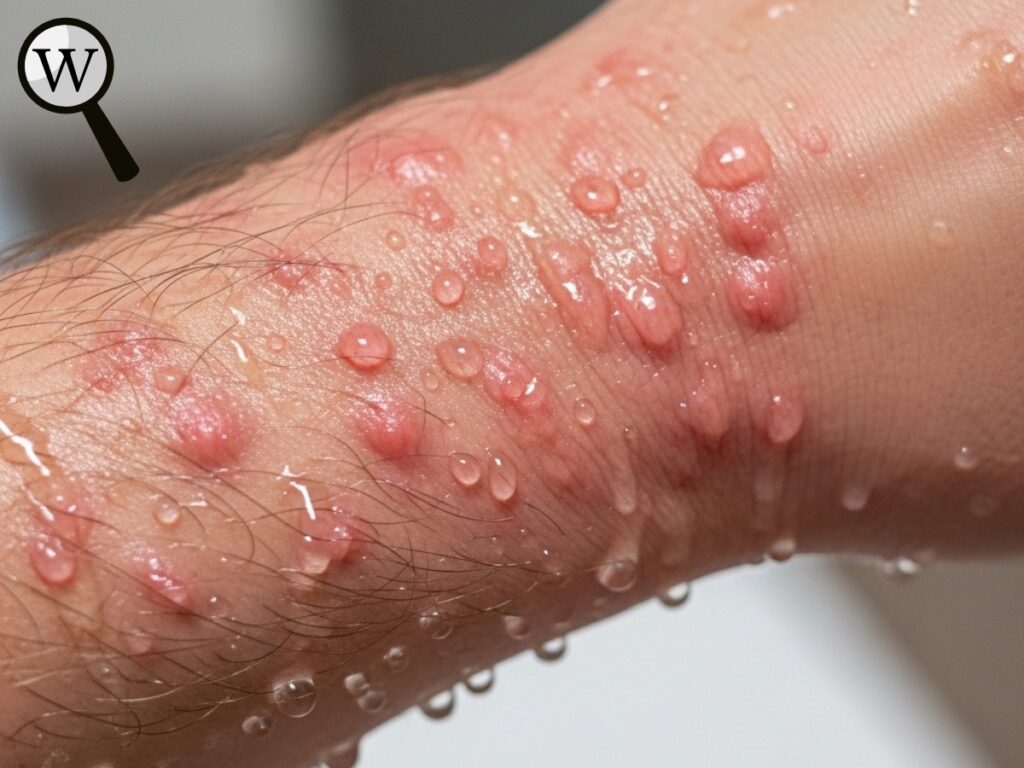
One of the most unimaginable rare diseases is aquagenic urticaria, a condition where contact with water—even one’s own sweat or tears—triggers painful hives and burning sensations. Only around 100 documented cases exist globally.
For those affected, taking a shower becomes a calculated risk, and exposure to rain or emotional crying can cause severe discomfort. Many manage their symptoms using antihistamines or phototherapy, but unfortunately, no definitive cure exists. The emotional and social toll is often as severe as the physical one.
Check more about Aquagenic urticaria on Wikipedia.
2. Solar Urticaria: Allergic to Sunlight

Another shocking condition is solar urticaria. Sufferers develop rashes, swelling, and intense itching within minutes of sun exposure. In severe cases, even short exposure can trigger systemic symptoms such as headaches, dizziness, or breathing difficulties.
To protect themselves, individuals with this disease often wear full-body UV-protective clothing, sunglasses, hats, and high-SPF sunscreens. Some must even avoid indirect sunlight or indoor lighting that emits UV rays. Treatment options include antihistamines, desensitization therapy, and in some cases, phototherapy to gradually build resistance.
The emotional toll is profound. Social isolation, restricted outdoor activity, and mental health struggles are common challenges for those affected.
Check more about Solar Urticaria from Cleveland Clinic.
3. Xeroderma Pigmentosum (XP): The Real ‘Children of the Moon’

Xeroderma Pigmentosum (XP) is a rare genetic disorder that dramatically increases sensitivity to ultraviolet (UV) rays. Even minimal exposure to sunlight can cause severe burns, DNA damage, and a dramatically elevated risk of skin cancer—sometimes appearing in early childhood.
Children with XP are often called “Children of the Moon” because they must avoid all sources of UV light, essentially living nocturnal lives. Daytime activities are heavily restricted unless strict protective measures are in place, including UV-blocking suits, visors, and indoor environments with filtered lighting.
While there is no cure, early diagnosis, lifestyle adaptations, and diligent medical monitoring can help extend life expectancy and improve quality of life. The name may sound poetic, but for these children and their families, it represents a life of vigilance, courage, and resilience.
Check more about Xeroderma pigmentosum from Derm Net.
4. Fibrodysplasia Ossificans Progressiva (FOP): The Human Statue Disease
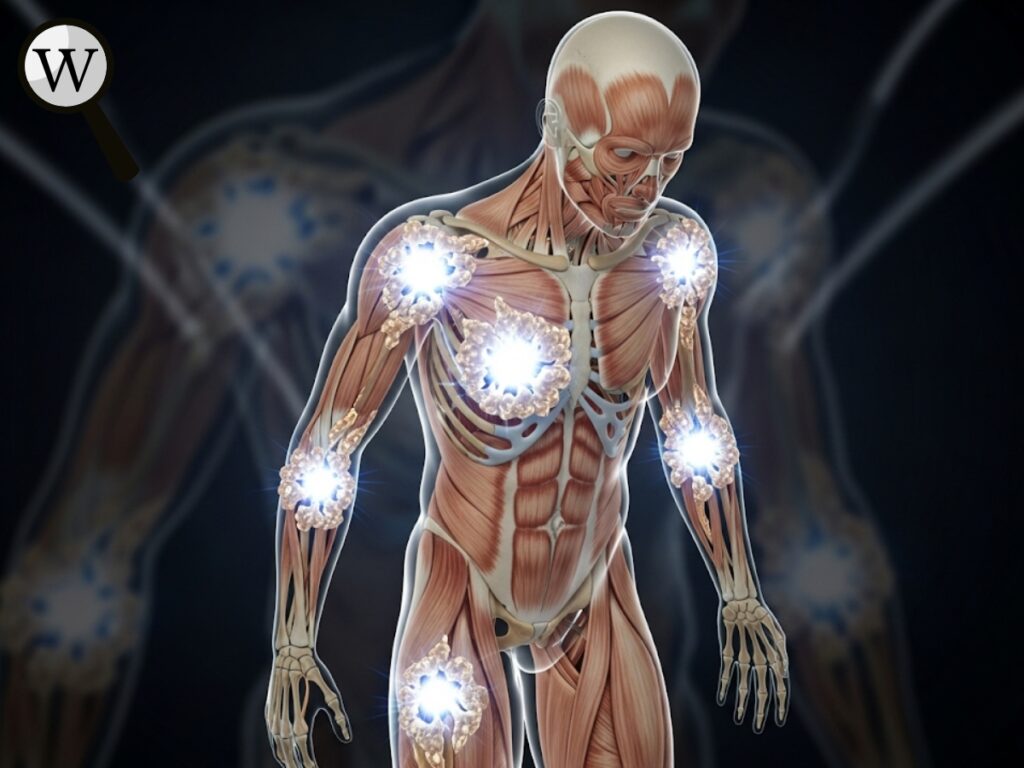
FOP is one of the most severe and disabling rare diseases known to medicine. It is an ultra-rare genetic disorder caused by a mutation in the ACVR1 gene, which leads the body to incorrectly turn soft connective tissues—like muscles, tendons, and ligaments—into bone. This abnormal bone growth, called heterotopic ossification, occurs progressively and unpredictably, forming a second skeleton that locks joints and restricts movement.
Even minor traumas, such as injections, falls, or muscle strains, can trigger new bone growth. The disease usually starts in early childhood, and most individuals lose mobility completely by early adulthood. There is currently no approved treatment or cure. Attempts to surgically remove the bone-like growths often result in even more aggressive regrowth. Research into genetic therapies and inflammation-targeting drugs is ongoing, offering hope for the future.
The psychological burden of FOP is profound. Many patients face progressive loss of independence, making assistive devices and full-time caregiving essential. Despite the challenges, individuals with FOP often become strong advocates and contributors to rare disease research, inspiring others with their resilience.
Check more about FOP from National Organization for Rare Disorders.
5. Hutchinson-Gilford Progeria Syndrome (HGPS): Rapid Aging
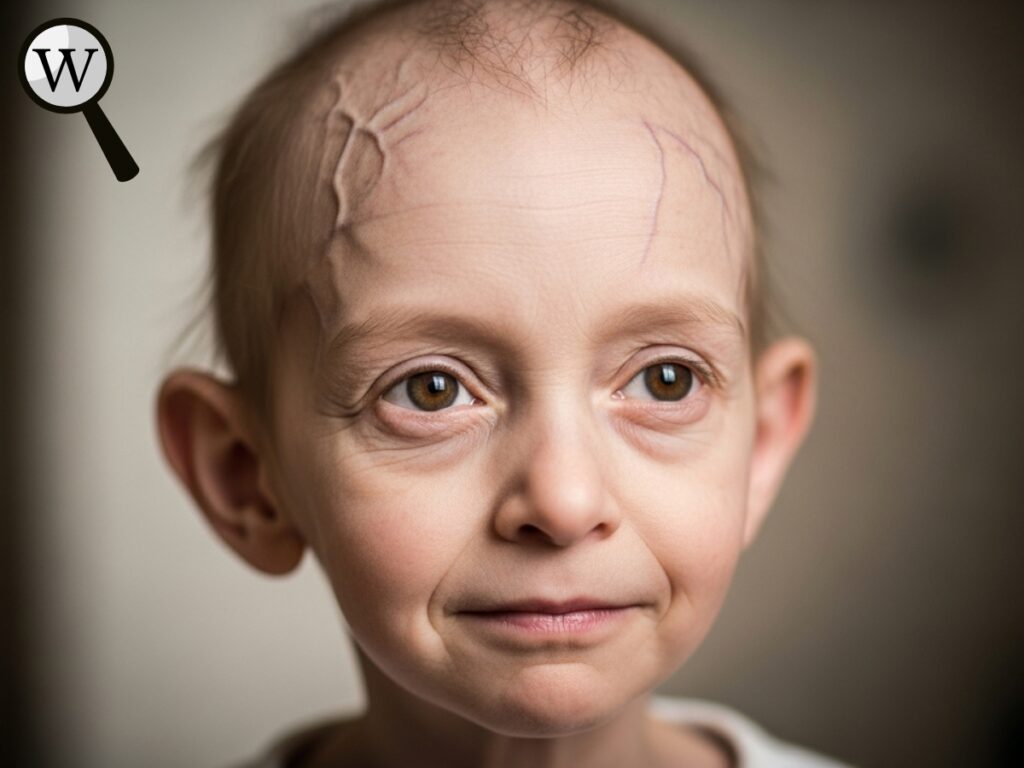
Children with HGPS, also known simply as progeria, experience symptoms of accelerated aging due to a mutation in the LMNA gene. This mutation produces an abnormal protein called progerin, which destabilizes the structure of the cell nucleus, leading to premature cell death and tissue dysfunction.
Symptoms typically begin to show between 12 and 24 months of age and include growth delays, hair loss, aged-looking skin, stiff joints, and cardiovascular problems. The most life-threatening complications are heart attacks or strokes due to hardened arteries. The average life expectancy for a child with HGPS is around 13 to 15 years.
While there is no cure, advancements in genetic research have led to the development of the first FDA-approved treatment—lonafarnib—a drug that can modestly extend lifespan and improve cardiovascular health. In addition to its devastating effects, HGPS has provided scientists with a unique window into the mechanisms of natural aging, potentially accelerating discoveries that may benefit the broader population.
Check more about HGPS from Childrens Hospital.
6. Non-24-Hour Sleep-Wake Disorder (Non-24)

Non-24-Hour Sleep-Wake Disorder, commonly referred to as Non-24, is an uncommon circadian rhythm disorder in which a person’s internal body clock does not synchronize with the natural 24-hour day-night cycle. Instead, their internal clock runs on a slightly longer cycle, causing their sleep and wake times to shift gradually later each day. This constant shift leads to periods of severe insomnia and intense daytime sleepiness, as their body’s internal schedule repeatedly clashes with societal demands like work and school.
The disorder is most prevalent in individuals who are completely blind because they lack the light cues needed to reset their biological clock daily. Light serves as the main environmental cue that helps align our internal body clock with the outside world. Without this crucial input, the body clock often defaults to its natural, slightly longer rhythm. While less common, this disorder can also affect sighted individuals, severely disrupting their daily functioning, social life, and work performance.
Although there is currently no cure for Non-24, various treatments aim to help regulate sleep patterns. These often include timed melatonin supplements or other medications designed to help the body’s clock realign with a 24-hour cycle. The goal of treatment is to reduce the chronic sleep disruption and its debilitating effects, allowing individuals to manage their schedules more effectively.
Check more about Non-24-Hour from Sleep Foundation.
7. Phenylketonuria (PKU)

Phenylketonuria, or PKU, is a genetic metabolic disorder caused by a deficiency in the enzyme phenylalanine hydroxylase. This enzyme is essential for breaking down the amino acid phenylalanine, which is a building block of protein found in most foods. Without this enzyme, phenylalanine accumulates to toxic levels in the blood and brain, causing serious health issues.
If left untreated, the buildup of phenylalanine can cause irreversible damage to the central nervous system, leading to severe intellectual disability, developmental delays, seizures, and behavioral issues. Early diagnosis is therefore critical to prevent these severe and permanent consequences. Today, newborn screening for PKU is standard practice in many countries, allowing for the condition to be identified and managed within the first few days of life.
The main treatment for PKU is a lifelong, strict diet that is very low in phenylalanine. This involves avoiding high-protein foods like meat, dairy, and nuts, and consuming special medical formulas that provide essential nutrients without phenylalanine. With careful and consistent dietary management, individuals with PKU can prevent brain damage and lead healthy, normal lives.
Check more about Phenylketonuria from Wikipedia.
8. Trimethylaminuria (Fish Odor Syndrome)

Trimethylaminuria is a rare metabolic disorder where the body cannot properly break down trimethylamine, a compound produced during the digestion of certain foods. Normally, a liver enzyme converts this compound into an odorless substance, which is then excreted. In individuals with this condition, this enzyme is either missing or not functioning correctly, causing an excess of trimethylamine to be released through sweat, urine, and breath. This results in a strong and unpleasant fish-like body odor.
The constant odor can have a devastating impact on a person’s quality of life. Many individuals with trimethylaminuria face significant social challenges, leading to embarrassment, anxiety, depression, and social withdrawal. They may be teased or bullied, and their condition can be misunderstood as poor hygiene. The emotional and psychological burden is often more challenging to manage than the physical symptoms themselves.
While there is no cure, the condition’s symptoms can be managed. The main strategy is a strict diet that avoids foods high in choline, a precursor to trimethylamine. These foods include marine fish, eggs, legumes, and certain meats. Good hygiene practices, along with specially formulated soaps and shampoos, can also help reduce the odor. In some cases, specific supplements or antibiotics may be prescribed to reduce the amount of odor-producing bacteria in the gut.
Check more about Trimethylaminuria from Metabolic Support Uk.
9. Allodynia

Allodynia is a neurological condition where a person experiences pain from stimuli that are not normally painful. The brain misinterprets harmless sensations, such as a light touch, a gentle breeze, or the pressure of clothing against the skin, as intense pain. This pain is often described as burning, aching, or searing. Allodynia is different from hyperalgesia, which is an exaggerated pain response to a painful stimulus.
Allodynia is not a disorder on its own but is a symptom of other underlying conditions. It is frequently seen in patients with fibromyalgia, diabetic neuropathy, nerve injuries, and migraines. The condition occurs when the central nervous system becomes sensitized, and the nerve pathways for touch and pain become tangled. This confusion in the nervous system means a simple touch can trigger a pain signal, making everyday activities debilitating.
Managing allodynia requires a comprehensive approach focused on treating the underlying cause. Treatment options include medications specifically for neuropathic pain, physical therapy to help desensitize the affected nerves, and, in some cases, nerve blocks. Because of its profound impact on a person’s daily life and quality of life, managing allodynia often requires a multidisciplinary team of healthcare professionals.
Check more about Allodynia from Lupus.
10. Congenital Insensitivity to Pain

Congenital insensitivity to pain is an extremely rare genetic disorder where an individual is born without the ability to feel physical pain. This condition is caused by mutations in specific genes that are responsible for the development and function of pain-sensing nerve cells. While the idea of not feeling pain might seem appealing, it is a life-threatening condition because pain is a crucial biological warning system that protects us from harm.
Without the ability to feel pain, individuals are vulnerable to repeated, often unnoticed, injuries, fractures, and burns. For example, a child with this disorder might not realize they have a broken bone or a severe burn, allowing the injury to worsen and become infected without immediate attention. This lack of a warning signal can lead to severe and life-threatening complications.
Managing this condition requires constant vigilance and proactive care. Individuals and their caregivers must regularly check for injuries, take preventive measures like wearing protective gear, and undergo frequent medical evaluations to detect problems early. Despite the dangers, with proper care and support, people with this condition can lead full and meaningful lives.
Check more about Congenital Insensitivity to Pain from BMJJournals.
Living with a Rare Disease: The Psychological Impact

Beyond the physical toll, rare diseases carry a profound emotional and psychological weight. Many patients endure years of misdiagnoses, often being told their symptoms are “all in their head,” leading to feelings of invalidation, confusion, and hopelessness. The journey to a proper diagnosis can stretch for years—sometimes decades—creating a cycle of frustration and anxiety.
Social isolation is another major challenge. Many rare diseases are visibly disfiguring, physically limiting, or misunderstood by peers and communities. This can lead to exclusion from school, work, or social life. Children may be bullied for looking or behaving differently, while adults might struggle to maintain careers or relationships due to the unpredictability of their condition.
Depression and chronic anxiety are common among both patients and caregivers. The uncertainty about the future, financial burdens of long-term care, and lack of available treatments amplify stress. Caregivers often experience “compassion fatigue” and need their own emotional support systems.
Thankfully, support networks are expanding. Online communities, nonprofit organizations, and rare disease foundations provide essential platforms for connection, education, and advocacy. Access to mental health professionals familiar with the unique needs of rare disease patients can also be transformative. Encouraging emotional wellness is not a luxury—it is a core part of comprehensive care.
Why Awareness Matters
Raising awareness of rare diseases does more than shine a light on overlooked conditions—it builds a sense of understanding and solidarity for the individuals and families affected. Awareness reduces stigma, fosters earlier diagnoses, and connects patients to vital resources and communities. It also plays a critical role in attracting scientific interest, research investment, and policy change. Every rare condition, no matter how obscure, holds clues that could unlock treatments or insights for more common diseases. In this way, raising awareness doesn’t just help the few—it paves the way for medical progress that benefits us all.
Final Thoughts
Life with a rare disease is more than just medical—it’s emotional, social, and deeply personal. These individuals are not just surviving; they’re showcasing unimaginable strength. Their stories remind us of the importance of compassion, awareness, and continued research in the fight against the unknown.
Want to discover more surprising facts? Explore our Facts section for endless fascinating insights!